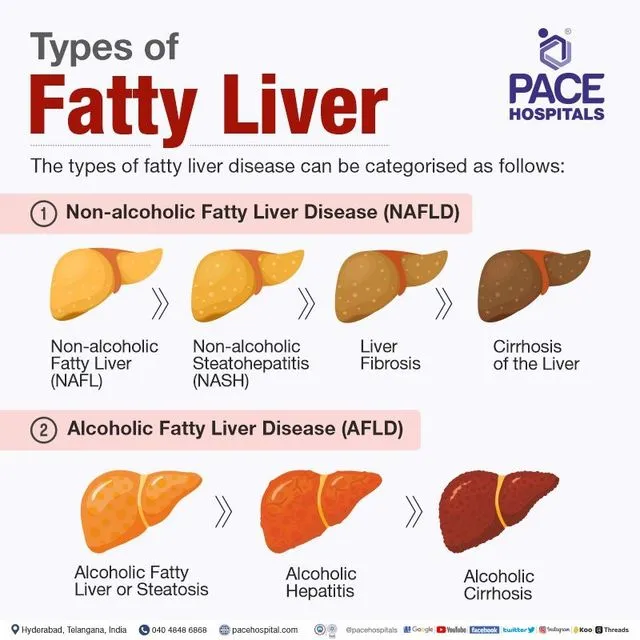
Fatty liver disease, also known as hepatic steatosis, is a condition in which excess fat builds up in the liver. This can lead to inflammation, scarring, and ultimately, liver damage. Fatty liver disease is becoming increasingly common, affecting approximately 25% of the global population. There are several factors that contribute to the development of fatty liver disease, including lifestyle choices, genetics, and underlying health conditions. In this article, we will break down the top contributors to fatty liver disease and discuss how to prevent and treat this condition.
1. Obesity
One of the leading causes of fatty liver disease is obesity. Excess body weight, particularly around the abdomen, can increase the risk of developing fatty liver disease. When the body has more fat than it can handle, the excess fat is stored in the liver, leading to the development of fatty liver disease. Losing weight through a healthy diet and regular exercise can help reduce the risk of fatty liver disease.
2. Poor Diet
A diet high in sugar, unhealthy fats, and processed foods can contribute to the development of fatty liver disease. These foods can increase the amount of fat in the liver and lead to inflammation and liver damage. Eating a balanced diet that is rich in fruits, vegetables, whole grains, and lean proteins can help prevent fatty liver disease.
3. Insulin Resistance
Insulin resistance is a condition in which the body’s cells do not respond properly to insulin, leading to high levels of glucose in the blood. Insulin resistance is closely linked to fatty liver disease, as it can increase the amount of fat stored in the liver. Managing insulin resistance through lifestyle changes, such as regular exercise and a healthy diet, can help prevent fatty liver disease.
4. Alcohol Consumption
Excessive alcohol consumption is a common cause of fatty liver disease. When alcohol is consumed in large amounts, it can lead to the accumulation of fat in the liver and inflammation. This can ultimately lead to alcoholic fatty liver disease, which can progress to more severe liver damage if left untreated. Limiting alcohol consumption or abstaining from alcohol altogether can help prevent fatty liver disease.
5. Genetics
Genetics can also play a role in the development of fatty liver disease. Certain genetic factors can increase the risk of developing fatty liver disease, even in the absence of other risk factors. If you have a family history of fatty liver disease, it is important to speak with your healthcare provider about ways to reduce your risk and monitor your liver health.
6. Medications
Certain medications can also contribute to the development of fatty liver disease. Medications such as corticosteroids, tamoxifen, and methotrexate can increase the amount of fat stored in the liver and lead to liver damage. If you are taking medications that may affect your liver health, it is important to speak with your healthcare provider about monitoring your liver function and exploring alternative treatment options.
7. Other Health Conditions
Certain health conditions, such as type 2 diabetes, high cholesterol, and metabolic syndrome, can increase the risk of fatty liver disease. These conditions can lead to insulin resistance, inflammation, and liver damage, all of which can contribute to the development of fatty liver disease. Managing these health conditions through lifestyle changes and medication can help reduce the risk of fatty liver disease.
Preventing and Treating Fatty Liver Disease
Preventing and treating fatty liver disease involves making lifestyle changes and addressing underlying health conditions. Here are some tips for preventing and treating fatty liver disease:
1. Maintain a healthy weight through diet and exercise.
2. Eat a balanced diet that is rich in fruits, vegetables, whole grains, and lean proteins.
3. Limit alcohol consumption or abstain from alcohol altogether.
4. Manage underlying health conditions, such as type 2 diabetes and high cholesterol.
5. Avoid medications that may affect liver health, if possible.
6. Speak with your healthcare provider about monitoring your liver function and exploring treatment options.
Frequently Asked Questions
Q: Can fatty liver disease be reversed?
A: In some cases, fatty liver disease can be reversed through lifestyle changes, such as losing weight, eating a healthy diet, and exercising regularly. However, in more severe cases, fatty liver disease can progress to more serious liver conditions, such as non-alcoholic steatohepatitis (NASH) or cirrhosis, which may require medical treatment.
Q: What are the symptoms of fatty liver disease?
A: Fatty liver disease often does not cause symptoms in its early stages. However, as the condition progresses, symptoms may include fatigue, weakness, abdominal pain, and jaundice (yellowing of the skin and eyes). If you experience any of these symptoms, it is important to speak with your healthcare provider for further evaluation.
Q: How is fatty liver disease diagnosed?
A: Fatty liver disease is typically diagnosed through a combination of blood tests, imaging studies (such as ultrasound or MRI), and a liver biopsy. Your healthcare provider may recommend these tests if they suspect you have fatty liver disease based on your symptoms and risk factors.
In conclusion, fatty liver disease is a common condition that can have serious consequences if left untreated. By understanding the top contributors to fatty liver disease and taking steps to prevent and treat this condition, you can protect your liver health and reduce your risk of liver damage. If you have concerns about fatty liver disease or would like more information, speak with your healthcare provider for personalized guidance and support.